Pericoronitis and Third Molar Surgery
It's exactly one week today since I had my right wisdom tooth out, surgically.
Looking at the mirror for the umpteenth time, I check to see how improved my face is and how much of the swelling had gone down.
Recently, I had to go under the knife, as a way to take care of the Chronic Pericoronitis I'd suffered.
What is Pericoronitis?
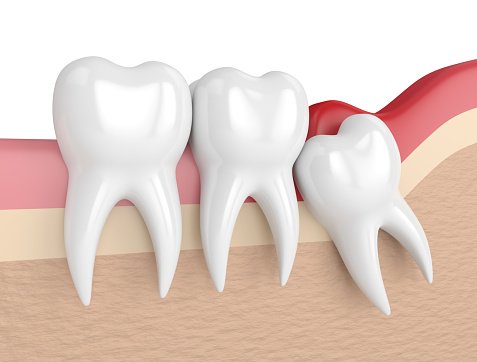
It is as the name implies, inflammation around the crown of a tooth.
It's a condition associated with impacted teeth of which commonly are canines and third molars, mostly mandibular third molars.
It's caused by limitation of space for eruption of teeth into the occlusal table.
Signs and Symptoms
This includes but not limited to:
- Pain
- Bleeding from the gum around the tooth
- Limitation in mouth opening (trismus)
- Pocket formation and food packing.
Types
This can be classified based on duration and severity into;
- Acute: of sudden onset, usually more painful and within a duration of 2 weeks and below.
- Subacute: In between acute and chronic, less than 4 weeks, more than 2 weeks.
- Chronic: low grade of pain, lasting more than 4weeks.
There's a variant, acute exacerbation of chronic pericoronitis. This is what is more common.
Management of Pericoronitis
Management starts with obtaining the right history, eliciting the signs and Symptoms and of course investigations.
A periapical or panoramic radiograph is the mode of investigation.
This helps to tell the type of pericoronitis based on the position of impacted tooth.
The position could be: vertical, mesioangular, distoangular or horizontal.
Removing the impacted tooth is the one sure method of treating Pericoronitis.
The other is to remove the inflammed gingival tissue around the crown of the tooth, in a process called operculectomy. This is less commonly done.
So, I had Pericoronitis, What Next?
I had an appointment with my senior colleague who's a surgeon and had a third molar surgery done. I stated how it was on the other side of the table.
Following the extraction, I've known pain like never before. The first 12hours post surgery, the pain and restlessness I felt was out of this world.
The swelling that ensued and the cascade of other reactions. This takes me to the complications of Third Molar surgery.
Complications of Third Molar Surgery:
Photo by Cedric Fauntleroy from Pexels
- Pain. This can be from dry socket or inflammation of the periodontal tissues of the adjacent teeth.
In my case, the latter was it. - Post surgical hemorrhage
- Swelling
- Limitation in mouth opening
- Nerve damage
- Abscess and infection
- Jaw fracture
I must have to say that this list of possible complications are not always the case.
In a week or two, the inflammation, swelling and pain is bound to resolve if the prescribed medication is taken adequately and the post op instructions taken seriously.
I'm getting quite relieved of the pain and working on the limitation of mouth opening so it doesn't progress to ankylosis.
I'll let you guys know how that goes, in time.
Source: from my knowledge (as trained) and more importantly from my personal experience as a patient 😂
And also from:
https://www.webmd.com/oral-health/guide/pericoronitis
https://pubmed.ncbi.nlm.nih.gov/31501778/
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2772836/
Thank you for reading.
Electronic-terrorism, voice to skull and neuro monitoring on Hive and Steem. You can ignore this, but your going to wish you didnt soon. This is happening whether you believe it or not. https://ecency.com/fyrstikken/@fairandbalanced/i-am-the-only-motherfucker-on-the-internet-pointing-to-a-direct-source-for-voice-to-skull-electronic-terrorism
Tooth surgery is one thing I dreaded the most because I've heard much bad news surrounding it. Thank goodness that you are fine now.
BTW, you might want to add references to your post so as to conform with the rules of the community.
Thank you.
I've conformed to the rules, sorry I overlooked it earlier.
Thank you for pointing it out.
Gracias.